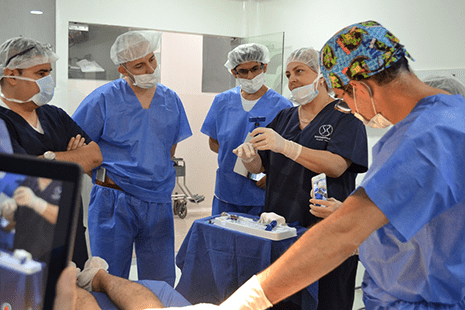
International Society for Stem Cell Application (ISSCA) and Marmara University Launch Stem Cell and Regenerative Medicine Fellowship Program in Turkey
Participants in the program will have access to over 200 hours of valuable online content and hands-on laboratory practice in the state-of-the-art facilities at Marmara University and StemBio. Generally, the program will cover a series of topics related to the general principles of regenerative medicine, including:
- Stem cell biology;
- Evidence-based treatments; and
- Tissue engineering.
Hear from Certified and Established Industry Leaders
The Stem Cell and Regenerative Medicine Fellowship Program aims to provide attendees with the chance to meet, interact, and learn from ISSCA-certified doctors, scientists, experts, and Marmara University professors with in-depth expertise in the field. There will be seven days of in-person training and a comprehensive digital course offering practical experience in stem cell classifications and laboratory applications, with a high emphasis on Good Manufacturing Practice (GMP) guidelines.
Learn About the Best Stem-Cell Application Practices and Procedures in Clinical and Manufacturing Operations
By attending the program, participants should be able to gain valuable answers to the “how to” questions related to the practical applications of stem cell biology and regenerative medicine in research laboratories and manufacturing facilities. Attendees can expect to learn the following:
- How to culture stem cells;
- How to meet quality control standards;
- How to comply with cGMP functions;
- How to operate within the recommended clinical procedures;
- How to apply and implement the regulations for stem cell processing in a certified manufacturing facility; and
- How to apply clinical guidelines and regulatory policies when developing a GMP facility
Besides, the seven-day fellowship program will also offer participants resources to bolster their stem cell operations, including copies of presentations, procedural guidelines, and all forms and documentation related to a GMP facility.
Moreover, the Stem Cell and Regenerative Medicine Fellowship Program will cover a range of clinical procedures, including:
- Tissue processing;
- Isolation of mesenchymal stem cells;
- Culture, Expansion and cryopreservation; and
- Clinical Application of stem cells for wide-ranging indications: participants will get case books and complete protocols for about 30 indications.
Why Attend the Stem Cell and Regenerative Medicine Fellowship Program?
The program provides a learning experience for medical professionals and scientists who’d love to further their knowledge and skills in stem cells and regenerative medicine. Attendees will get the opportunity to learn from the top professionals in the field and gain practical hands-on experience in world-class laboratory facilities.
Here’s what Global Stem Cells Global’s CEO, Benito Novas, had to say: “We are delighted to hold the Stem Cells and Regenerative Medicine Fellowship Program, which is designed to provide participants with the opportunity to gain and further their knowledge in stem cell biology and tissue engineering. In addition, ISSCA’s partnership with Marmara University will ensure attendees have access to professors with deep knowledge in the field and practical training in stem cell and regenerative medicine.”
For more information on the Stem Cell and Regenerative Fellowship Program, visit the ISSCA website or contact Global Stem Cells Group.
About Marmara University
Marmara University is a leading research university nestled in Istanbul, Turkey. It’s a distinguished academic institution with high authority in scientific research and academic excellence, specifically in medicine. The university provides undergraduate, graduate, and doctorate degrees, as well as certificate programs. Marmara University also boasts state-of-the-art facilities and dedicated faculty that chronicle its dedication to giving scholars world-class learning experiences and contributing to the advancement of knowledge in wide-ranging fields.
About ISSCA:
The International Society for Stem Cell Application (ISSCA) is a multidisciplinary community of scientists and physicians who aspire to treat diseases and lessen human suffering through advances in science, technology, and the practice of regenerative medicine. ISSCA serves its members through advancements made in the specialty of regenerative medicine.
The mission of the International Stem Cell Certification Agency (ISSCA) is to establish itself as a global leader in regenerative medicine certification, education, research, and training.
ISSCA provides certification training in cities worldwide because it recognizes the importance of standards and certifications in regenerative medicine as a medical specialty. To help more people, both locally and globally, as the demand for more doctors interested in and comfortable with regenerative medicine surges. ISSCA’s mission is to advance quality and uniformity in regenerative medicine worldwide.
About Global Stem Cells Group:
The Global Stem Cell Group is a family of several companies focused on stem cell medicine and research. The company uses its network to bring leadership in regenerative medicine training, research, and patient applications.
GSCG’s mission is to allow physicians to present the benefits of stem cell medicine to patients worldwide. The company also partners with policymakers, educators, and regulators to promote regenerative medicine.
Global Stem Cells Group is a publicly traded company operating under the symbol MSSV. https://finance.yahoo.com/quote/mssv/
To learn more about Global Stem Cells Group, Inc.’s companies visit our website www.stemcellsgroup.com or call +1 305 560 5331
Safe Harbor Statement:
Statements in this news release may be “forward-looking statements”. Forward-looking statements include, but are not limited to, statements that express our intentions, beliefs, expectations, strategies, predictions, or any other information relating to our future activities or other future events or conditions. These statements are based on current expectations, estimates, and projections about our business based partly on assumptions made by management. These statements are not guarantees of future performance and involve risks, uncertainties, and assumptions that are difficult to predict. Therefore, actual outcomes and results may and are likely to differ materially from what is expressed or forecasted in forward-looking statements due to numerous factors. Any forward-looking statements speak only as of the date of this news release, and The Global Stem Cells Group undertakes no obligation to update any forward-looking statement to reflect events or circumstances after the date of this news release. This press release does not constitute a public offer of any securities for sale. Any securities offered privately will not be or have not been registered under the Act and may not be offered or sold in the United States absent registration or an applicable exemption from registration requirements.
- Published in News
Stem Cell Center Network in Lisbon Portugal
The Stem Cell Center Network ( a Division of Global Stem Cells Group ) is an international network of regenerative medicine practitioners . Dedicated to promoting the research and development of the field of regenerative medicine, and strives to bring patients cutting-edge treatments that make use of the ever-growing list of benefits that regenerative medicine carry. This week, in a part of their effort to expand their foothold in medical communities around the world, the Stem Cell Center Network has announced the opening of a new training facility in Lisbon, Portugal.
Over the years, the Stem Cell Center Network has sought out to aggressively expand and roll out new membership opportunities, programs, events, and more– an effort that has been redoubled in the last five years. As a result, we have added members that practice regenerative medicine under our banner in over twenty five countries spread across five continents.
The new Portuguese center will be located in the clinic of Dr. Hugo Madeiras, a highly-accredited physician and scientist who will preside over the facility as the Global Stem Cells Group chief representative in Portugal. As the CEO and founder of the Clinic of Advanced Implantology, he focuses exclusively on implantology, esthetics, and digital workflows, and collaborates with over twenty doctors and seventy resources in total. He is also the clinical collaborator for the Straumann Group, a faculty which includes product testing, lecturing, and the creation and delivery of educational content.
Dr. Madeiras graduated from the Instituto Superior de Ciências da Saúde Egas Moniz in Medicine in 2007, and with a Master in Oral Rehabilitation from CESPU in 2009. With his over ten year of experience in the field, he acts as a speaker at several national and international congresses that go over developments and new treatment protocols in the field of dentistry.
“This new center will help in bringing regenerative medicine to the people of Lisbon. It will treat patients with a wide variety of different diseases, but with a special emphasis on Aesthetic Medicine,” Said Benito Novas CEO of the Global Stem Cells Group about the new Stem Cell Center Network partnership, “This new facility will be at the top of the line, a place where Portuguese doctors can come to learn about regenerative medicine protocols, and the advancements that have been made in the field. I am incredibly excited to be working in partnership with Global Stem Cells Group , and look forward to many years as a program leader here in Portugal,”
Stem Cell Center Network plans for the clinic to open in September 2020– and with that date looming closer and closer with each passing week, a date has also been agreed upon for the clinic’s inaugural training– indeed, it will be a place for doctors around the country to convene and learn, share, and research the complexities and applications of regenerative medicine. Barring any extenuating circumstances, the next first Regenerative Medicine Certification Training in the Portuguese clinic will take place on September 25 & 26th, 2020– just weeks after its formal opening. With only 10 spots available, applicants are encouraged to sign up soon for the hands-on training course.
To sign up today, visit: https://issca.us
About Global Stem Cells Group
Global Stem Cells Group (GSCG) is a worldwide network that combines seven major medical corporations, each focused on furthering scientific and technological advancements to lead cutting-edge stem cell development, treatments, and training. The united efforts of GSCG’s affiliate companies provide medical practitioners with a one-stop hub for stem cell solutions that adhere to the highest medical standards.
Global Stem Cells Group is a publicly traded company operating under the symbol MSSV.
https://finance.yahoo.com/quote/mssv/
- Published in News
Can Stem Cells treatment Regrow the knee cartilage?
Some people believe that stem cells can achieve this, but studies show it’s unlikely in most cases. While minimal growth may be observed a year after treatment, full cartilage replacement is rare.
Limited Regenerative Capacity of Cartilage
Cartilage has limited regenerative capacity, and current pharmacological treatments offer only symptomatic relief. Patients who don’t respond to conventional therapies may undergo surgical procedures like arthroplasty or total joint replacement.
Stem Cells for Cartilage Repair
Stem cells from various tissues have been used over the last two decades to treat osteoarthritis and bone damage. They primarily aid in cartilage repair but often fail to fully replicate native tissue properties.
Potential of Stem Cell Therapies
Stem cell therapies using MSCs or iPSCs have shown promise in clinical settings. iPSCs, in particular, offer patient-specific regeneration potential.
Understanding Cartilage and Its Damage
Cartilage is crucial for joint function, providing cushioning and flexibility. Damage, whether from trauma or conditions like osteoarthritis, reduces its effectiveness.
Treatment Options for Cartilage Damage
Current treatments focus on symptom relief or joint replacement for severe cases.
How Stem Cells Can Help
Stem cells, sourced from bone marrow or fat, can develop into chondrocytes and aid in reducing inflammation and stimulating repair.
Challenges in Cartilage Regrowth
Cartilage’s complex structure requires more than just cell injection for effective regeneration. Scaffold-like structures are being researched for better outcomes.
Mechanism of Stem Cell Action
Stem cells work through anti-inflammatory processes and regeneration stimulation, though they do not transform into different tissues.
Role of ISSCA in Advancing Regenerative Medicine
The ISSCA promotes standards and research in regenerative medicine, offering certifications and advancing the field’s understanding.
- Published in Blog
Platelet-Rich Plasma Stays Quietly Popular Despite Neglect
Introduction
FRIDAY, 27 APRIL 2018 / PUBLISHED IN BLOG
Fact: PRP Treatments in High Demand
According to research, PRP treatments are one of the most in-demand treatments available in healthcare. This is impressive considering the following:
- PRP is not supported by the medical industry. No big pharma funding on extensive research or marketing. No medical associations lobbying to increase its awareness.
- PRP is shunned by the insurance companies. No reimbursements from them. So getting patients to pay is difficult, especially for a treatment that’s relatively “unproven” like this.
- The cost of PRP treatments is actually rising. In 2006, you could get a PRP treatment for $450. Today it costs $800. The cheapest we’ve seen is $650. The prices are still robust as demand keeps up.
The Future Potential of PRP
We believe the best of PRP is not even here yet. We’re just one breakthrough study away from exploding into mainstream hospitals and clinics. We see the biggest growth in Platelet-Rich Plasma happening in Asia.
Strongly Based on Fundamental Healing Theory
The growth can be attributed to PRP’s fundamental healing property. More platelets. More growth factors and cytokines. And therefore more healing. It’s as simple as that. And no one can argue this fact.
Our body’s natural healing mechanism operates with 150,000/ul-350,000/ul platelets in blood. Using Platelet-Rich Plasma means this number is amplified by 3X to 5X. How can this not translate into better healing?
Believe it or not, the best orthopedic doctors use Platelet-Rich Plasma regularly.
PRP’s Applications and Effectiveness
PRP can be used to promote healing of injured tendons, ligaments, muscles, and joints and can be applied to various musculoskeletal problems. They conduct regular studies to test its effectiveness.
Key Study on PRP and Chronic Low Back Pain
One landmark study involved double-blind randomized controlled trials to see the effect of PRP on patients with chronic low back pain caused by torn discs. The study outcome says 60% of the patients felt significant improvements. Some were cured.
Different Variants of Platelet-Rich Plasma
So far, there are the following types of PRP variants:
- Plasma Rich in Growth Factors (PRGF)
- Plasma Rich in Platelets and Growth Factors (PRPGF)
- Platelet-Rich Plasma (PRP); Platelet Poor Plasma (PPP)
- Plasma Rich in Platelets and Rich in Leukocytes (LR-PRP)
- Plasma Rich in Platelets and Poor in Leukocytes (LP-PRP)
- Platelet-Rich Fibrin Matrix (PRFM)
All of them involve plasmapheresis — the two-stage centrifugation process to separate platelets from blood. However, what happens after that can be different. The industry hasn’t found its middle ground as to which variant to be standardized. We believe the confusion will clear up in 3-5 years.
Bio-Factors at Play in PRP
No matter which variant you end up using, the bio-factors at play are the following:
- Growth factors: TGF-B, PDGF, IGF-I, II, FGF, EGF, VEGF, ECGF
- Adhesive proteins: Fibrinogen, Fibronectin, Vitronectin, Thrombospondin-1
- Clotting & Anti-Clotting factors: Proteins, Antithrombin, Plasminogen, Proteases, Antiproteases
How Platelet-Rich Plasma Actually Works
Why is the treatment commonly used for wound healing and pain management? The answer is because the platelets’ main job is to aid coagulation, act as a biological glue, and support stem or primary cell migration. In addition, it also helps in restoring hyaluronic acid and accelerates the synthesis of collagen and glycosaminoglycans, increasing the cartilage matrix.
Not only that, the platelets are delivered in a clot, which means it can immediately act as a scaffold to enable the healing process. 95% of the bio-active proteins are released within 1 hour of injecting Platelet-Rich Plasma. The platelets continue to release growth factors for 7-10 days. Thus it’s recommended to re-inject PRP every 7 days.
Patient Perspective on PRP Costs
Why are patients coughing up their hard-earned money for this?
This reminds me of hundreds of thousands of PRP treatments paid from patients’ own pockets even though they’ve been paying for years to get covered by their respective insurance providers. In 2015, PRP costs were anywhere between $600 and $800 per site per treatment. And most patients go for repeated treatments. So why were they forking up their hard-earned money if the treatment was not working? Weren’t there any better alternatives under the “coverage” of their insurance provider? The answer is 1) the treatment works. 2) there’s nothing else out there that’s as natural and side-effect-free as PRP.
PRP and Osteoarthritis
Consider the case of osteoarthritis. 27 million Americans are impacted by it. 33.6% of people older than 65 are victims. All of them experience gradual degeneration of cartilage and bones — they lose roughly 5% of cartilage per year. Yet, our medical industry doesn’t have a fix to stop it.
However, when doctors started doing PRP treatments for their osteoarthritis patients, they found a large majority of them had no further cartilage loss. To me, it means we should make PRP treatments the default first-line treatment for osteoarthritis across the country.
PRP in Hair Loss and Cosmetic Applications
Another huge market is hair loss and cosmetic facial applications. I know there are many people who believe PRP doesn’t work for hair. Here’s what one of the Platelet-Rich Plasma studies found were the effect of the treatment on hair loss.
“Hair loss reduced and at 3 months it reached normal levels. Hair density reached a peak at 3 months (170.70 ± 37.81, P < 0.001). At 6 months and at 1 year, it was significantly increased, 156.25 ± 37.75 (P < 0.001) and 153.70 ± 39.92 (P < 0.001) respectively, comparing to baseline. Patients were satisfied with a mean result rating of 7.1 on a scale of 1-10. No remarkable adverse effects were noted.”
I’ll take that. That’s me getting PRP for hair.
PRP Market Growth
The PRP market is expected to hit $126 million in 2016. That number looks paltry. But that’s a 180% increase over the 2009 figure of $45 million.
Consider this. Just for osteoarthritis alone, if all the 27 million Americans receive 1 PRP shot a year at a conservative $400 per treatment, it would be a market of $10 billion. And that’s one condition out of the many that Platelet-Rich Plasma injections are proven to work.
PRP and Tennis Elbow
Another condition that PRP is known to work very well is Tennis Elbow. It affects on average 1% to 3% of the overall population. That number is as high as 50% among tennis players.
Insurance Coverage and PRP
Just getting Platelet-Rich Plasma covered by insurance will unleash the market big time and will help heal millions of patients naturally, more effectively.
Oh ya, that means the insurance companies will have to pay more. Why would they?
Potential Savings for Insurance Companies
HOWEVER, if this treatment could reduce further expensive intervention like surgery, then it may actually be a blessing for the insurance guys in terms of savings. One surgery avoided by a patient through the right intervention through PRP treatments will save the insurance companies at least $25,000. Now, that’s a win-win for both patients and insurance.
I believe it’s a matter of time before insurance companies start realizing their folly of not supporting this treatment.
PRP Still Considered “Unproven”
After all is said and done, it’s still “unproven.” The problem with PRP is that it can be used for just about everything, which is a good problem to have until healthcare officials (and insurance companies) start realizing that people are going to misuse it.
So it’s classified as unproven. The VAST scope of the treatment calls for urgent structure and guidelines. There are some 20+ conditions where researchers have found it “helps” in one way or another. It’s a daunting task to prove its efficiency in all the areas. Nevertheless, we’ll get there. Though we’ll need a lot of funding for that.
Need for Standardization
And yes, we need to standardize the procedure. As well as come up with optimized protocols for each condition. Someone needs to take initiative on that. We’re counting on independent doctors and medical institutions. The big pharma won’t jump in because what’s in it for them, right?
Simplicity and Accessibility of PRP
It’s so simple, you’d be an idiot not to try it. You only need a vacuum blood harvesting tube like what we offer here, a centrifuge with an adapter for the tube, pipettes, and 10ml ampules of 10% calcium chloride.
The only complexity comes from not following a standard PRP system. Because the final platelet count can depend on a variety of factors like the initial volume of blood, the technique used, and the relative concentration of WBC and/or RBC. As well as on the patient’s side, there are factors such as age.
- Published in Blog
The Growth Factor Showdown: Plasma Vs Fibrin
WEDNESDAY, 25 APRIL 2018 / PUBLISHED IN BLOG
Platelet-Rich Plasma (PRP) and Platelet-Rich Fibrin (PRF) have been the subject of numerous speculations regarding their efficacy in facilitating angiogenesis, hemostasis, osteogenesis, and bone growth. The primary reason these platelet products are effective is due to the growth factors they carry. Let’s delve into the specific roles of these growth factors in the healing process.
Growth Factors in Platelet-Rich Plasma
These growth factors play vital roles in PRP and contribute significantly to the healing process:
Platelet-Derived Growth Factor (PDGF)
Regulates cell growth and division, especially in blood vessels, making it crucial for blood vessel reproduction.
Transforming Growth Factor Beta (TGF-β)
Responsible for overall cell proliferation, differentiation, and various other cellular functions.
Fibroblast Growth Factor (FGF)
Plays a key role in wound healing and embryonic development, influencing the proliferation and differentiation of specialized cells and tissues.
Vascular Endothelial Growth Factor (VEGF)
Essential for vasculogenesis and angiogenesis, VEGF restores oxygen supply to cells when it is inadequate and helps create new blood vessels after injury.
Keratinocyte Growth Factor (KGF)
Found during the epithelialization phase of wound healing, KGF stimulates the formation of epithelium immediately after a wound or injury occurs.
Connective Tissue Growth Factor (CTGF)
Functions in cell adhesion, migration, proliferation, angiogenesis, skeletal development, and tissue wound repair.
Platelet-Rich Plasma Rules
A recent study suggests that PRP and its gelled cousin, PRF, differ significantly in the release of these growth factors, which can affect the healing outcome. The study concludes that:
PRP releases significantly higher proteins at earlier time points, which is beneficial for short-term effects.
PRF shows a continual and steady release of growth factors over a 10-day period, making it more beneficial for long-term healing.
Advantages of Platelet-Rich Fibrin Over Platelet-Rich Plasma
PRF has some notable advantages over PRP, including:
- It doesn’t require thrombin and anticoagulants.
- It results in better healing due to its slow polymerization process.
- It aids in hemostasis.
How Platelet-Rich Plasma Differs from Platelet-Rich Fibrin
Platelet-Rich Plasma is produced using a double spin method: a hard spin to separate red blood cells from everything else in the autologous blood, followed by a soft spin to separate the platelets and white blood cells, resulting in PRP, Platelet-Poor Plasma (PPP), and Red Blood Cells.
Platelet-Rich Fibrin is created using a newer method. After the first centrifugation, the middle layer is taken, containing fewer platelets but more clotting factors. This gradually forms into a fibrin network that traps cytokines and is then centrifuged again to result in PRF, a fibrin layer containing platelets and plasma.
What Matters in Healing
When it comes to accelerating healing, the immediate availability of growth factors and cytokines is crucial. PRP may be more effective in this regard due to its immediate release of growth factors, allowing for repeated injections for additional healing factors just days after the initial injection.
Conclusion
Platelet-derived products are still in their infancy. Despite their potential benefits, more research is needed to fully understand their capabilities. If you’re a physician using any or both of these products, we encourage you to share your experiences with us through our contact form.
- Published in Blog
Platelet-Rich Plasma For Breast Augmentation: How it works
FRIDAY, 20 APRIL 2018 / PUBLISHED IN BLOG
“You start out happy that you have no hips or boobs. All of a sudden you get them, and it feels sloppy. Then just when you start liking them, they start drooping.”
— Cindy Crawford
Just like men associate (some of) their masculinity with the shape and size of their muscles, women associate (some of) their femininity with the shape and size of their breasts. However, unlike muscles, exercise won’t help augment the size of breasts. Fortunately, there are various procedures available, and today, we’ll explore how Platelet-Rich Plasma (PRP) can aid in breast augmentation.
Platelet-Rich Plasma for Breast Augmentation
PRP and Breasts: The Incorrect Perception
Currently, traditional breast augmentation procedures like breast implant surgery and fat grafting are the most effective methods. However, the general public often misunderstands PRP’s role in breast augmentation. Here’s a typical conversation between a patient and a dermatologist:
Patient: “Hey, I heard about this thing called PRP, and I was told it’s just a couple of injections with stuff drawn from our own blood.”
Doctor: “Yeah, they are really good.”
Patient: “Really? You think so? I also heard they’re good for breast augmentation. Can you do it for me?”
This is usually followed by the doctor explaining how PRP is a healing tool, not an implant tool.
How Platelet-Rich Plasma for Breast Augmentation Works
PRP can be used in two primary ways for breast procedures:
Fat Transfer and Platelet-Rich Plasma for Breast Lift
Fat transfer involves taking unwanted body fat via liposuction from other parts of the body and processing it before injecting it into the upper part of the breast and cleavage area. This provides immediate enhancement. However, the sudden expansion can cause blood vessels to block, leading to sensitivity loss in some parts of the breasts or nipples.
To avoid this, it’s best to ensure sufficient collagen and growth factors are supplied. This is where PRP comes in. The doctor adds PRP, derived from the patient’s own blood, to the fat during processing. The end product, containing many blood-derived growth factors and collagen for skin rejuvenation, is then injected like a typical PRP injection. The result is firmer breasts with changes in size, skin texture, and breast shape, without sensitivity loss. Some call this procedure the Platelet-Rich Plasma Facelift. Results generally last from 9-18 months.
This procedure boosts the confidence of many women but is not recommended for those with:
- Extreme loss of volume
- Excessive sagging
- Previous breast implants
Only Platelet-Rich Plasma for Breast Rejuvenation
This procedure is purely for rejuvenation. It’s for women satisfied with their breast size but looking to rejuvenate the skin, restore fullness, and regain sensitivity. The process involves drawing 20ml of the patient’s blood, spinning it twice in a tabletop centrifuge, and then injecting it into the necessary areas. PRP injections not only enhance appearance but also produce new tissues, resulting in better cleavage and fullness.
Additional Perks
Some professionals believe that traditional breast implants by a board-certified plastic surgeon are the gold standard. However, natural methods like PRP are becoming the new gold standard. Unlike artificial implants, PRP does not require cutting into the breasts, which means no scars and no need for replacement after 10 or 20 years.
“It wasn’t just her beauty. It was the attitude in her smile, the tilt of her head, and the loving look in her eyes when she caught me sneaking a peek down her shirt.”
— John L. Monk, Kick
By structuring the article with H2 headings and enhancing readability, this version should be more engaging for readers and better optimized for search engines.
- Published in Blog
Platelet-Rich Plasma For Bone Healing: Myth or Fact?
WEDNESDAY, 11 APRIL 2018 / PUBLISHED IN BLOG
Platelet-Rich Plasma (PRP) has a proven record for healing soft tissues and other living tissues. But can it actually heal bones? This could mean PRP, when applied to an affected area such as an elbow joint, knee, or backbone area, heals everything within its reach, including bones. Is that really why PRP works? Let’s examine.
Platelet-Rich Plasma for Bone Healing
Bones are not just lifeless matter attached to living tissues. They are as much living as the tissues themselves and are constantly changing. Old bone cells are broken down and replaced with new ones in a three-part process called bone remodeling. This involves resorption (digestion of old bone cells), reversal (birthing of new cells), and formation (new cells turn into fully formed bones).
This process, like other biological processes in the body, requires hormones and growth factors. Some of these include parathyroid hormone (PTH), calcitriol, insulin-like growth factors (IGFs), prostaglandins, tumor growth factor-beta (TGF-beta), bone morphogenetic proteins (BMP), and cytokines. For this discussion, we need to remember only one thing: a large number of cytokines and growth factors are involved in the bone remodeling process. This means we can accelerate the bone remodeling process by supplying these cytokines and growth factors as suggested by various studies.
Why Platelet-Rich Plasma?
Autologous Platelet-Rich Plasma (PRP), being completely “whole and natural,” can more closely simulate a highly efficient in-vivo situation than anything else made up of artificial recombinant proteins. In PRP, we take advantage of the biological benefits of growth factors whose functions we know as well as those we do not know yet. From the 15+ factors we know are in PRP, including platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-beta), platelet factor 4 (PF4), interleukin 1 (IL-1), platelet-derived angiogenesis factor (PDAF), vascular endothelial growth factor (VEGF), epidermal growth factor (EGF), platelet-derived endothelial growth factor (PDEGF), epithelial cell growth factor (ECGF), insulin-like growth factor (IGF), osteocalcin (Oc), osteonectin (On), fibrinogen (Fg), vitronectin (Vn), fibronectin (Fn), and thrombospontin-1 (TSP-1), we’re supplying a “holistic” set of nutrients for healing that cannot be mimicked by those obtained artificially.
PRP: Organic Fertilizers for the Body
The difference with PRP is akin to adding chemical fertilizers versus organic fertilizers to plants. Chemical fertilizers are rich in essential nutrients that we know are needed for crops. On the other hand, organic fertilizers supply nutrients not only to the plants but also to the soil, improving the soil structure and tilth, water-holding capacity, reducing erosion, and promoting slow and consistent release of nutrients to the plants. Clearly, organic fertilizers are better, aren’t they?
Platelet-Rich Plasma is like organic fertilizers for our body.
Bonus: Strong Antimicrobial Properties
PRP’s healing function also has synergistic antimicrobial properties. A new study confirms that using Platelet-Rich Plasma in surgeries may have the potential to prevent infection and reduce the need for costly post-operative treatments. That’s a nice bonus for the organic fertilizer of our bodies. Perhaps there are more benefits to discover.
Conclusion
The scope of Platelet-Rich Plasma is growing as the scientific community continues to unearth its inherent properties. PRP is an unignorable and unavoidable component of healing.
- Published in Blog
Why Should you Include PRP In Your Medical Practice?
MONDAY, 26 MARCH 2018 / PUBLISHED IN BLOG
Platelet-Rich Plasma (PRP) has been a lifesaver for many medical practices, reigniting physicians’ passion for medicine. Not only is it 100% derived from the patient’s own body, but it is also natural and comes with minimal side effects. PRP can treat a wide range of medical conditions, often outperforming other treatment options.
The Simplicity of PRP
One of the most compelling reasons to include PRP in your practice is its simplicity. With an initial investment of about $1000, you can start offering PRP therapies. The equipment is relatively inexpensive and pays for itself quickly.
Long-Term Popularity
PRP is not a passing trend. It has been gaining popularity for years and shows no signs of slowing down. The market for PRP therapies is expected to reach nearly $500 million within the next decade, with an annual growth rate of 12.5% since 2015.
High Patient Satisfaction
Patient satisfaction is another significant advantage. In certain cases, satisfaction rates have been as high as 95%. Patients are often surprised by the efficacy of PRP, believing that their conditions could not be reversed or halted without side effects, downtime, and invasive surgeries.
Meeting the Growing Demand
Now is the time to start including PRP in your practice. The supply is low, but demand is booming. PRP therapies hold great promise, especially when combined with other treatments to increase efficacy. Since no standard has been established, you have the opportunity to set these standards yourself.
Be a Pioneer in PRP Therapy
It is vital that more doctors utilize PRP therapy to become pioneers in this field. PRP has the potential to revolutionize medicine, and missing out would not be a smart option.
Versatility Across Specialties
PRP can be utilized in almost every field and specialty, from sports medicine and pain management to skin rejuvenation, hair care, and even urology. Most physicians who use PRP treatments have also seen higher patient retention rates.
Conclusion: A Smart Addition to Your Practice
So, is there a legitimate reason not to add PRP to your practice? With its simplicity, high patient satisfaction, growing popularity, and versatility, PRP is a smart addition to any medical practice. Start offering PRP treatments and watch your practice thrive.
- Published in Blog
How To Choose A Platelet-Rich Plasma (PRP) Kit
MONDAY, 26 MARCH 2018 / PUBLISHED IN BLOG
Platelet-Rich Plasma (PRP) extraction methods have sparked debate due to varying reliability. Understanding how to select the best PRP kit can resolve these concerns and optimize treatment outcomes.
The Importance of Using a PRP Kit
Merely centrifuging blood in a test tube—often termed “bloody PRP”—is ineffective and may contain excessive red and white blood cells, potentially causing post-injection flare-ups. In contrast, PRP kits can concentrate platelets up to 5-7 times baseline levels, crucial for effective treatment.
Characteristics of a Good PRP Kit
Choosing the right PRP kit hinges on its ability to control platelet concentrations and eliminate unwanted cells, tailored to specific medical conditions.
Gel Separators
Kits with gel separators separate blood components via osmosis, retaining plasma and platelets while removing red and white blood cells. This method achieves modest platelet concentrations.
Buffy Coat
PRP kits that feature a buffy coat layer offer higher platelet concentrations (5-7 times baseline). The buffy coat, composed of platelets and white blood cells, is separated from red blood cells to minimize contamination.
Buffy Coat with Double Spin
Optimal for PRP quality, this kit further purifies the buffy coat by eliminating red blood cells through a second spin. This results in highly concentrated PRP with minimal red blood cell presence.
Biosafe Kit
Regarded as one of the best on the market, the Biosafe kit provides precise control over PRP production. It yields approximately 10cc of product, which can be double-spun for optimal platelet concentration. Users can customize the final product by choosing the inclusion or exclusion of red blood cells.
Understanding Leukocyte-Poor PRP
Leukocyte-poor PRP excludes white blood cells, which some believe may trigger inflammation and hinder growth factors. However, others argue that leukocytes are crucial for healing responses, promoting tissue regeneration and enhanced growth factor presence.
Choosing Filters for Leukocyte Reduction
To achieve leukocyte-poor PRP, practitioners can utilize Leukocyte Reduction (LR) filters like the CIF-LR filter, which efficiently separates white blood cells via electrostatic attraction. This ensures minimal clogging and filters out up to 99.99% of white blood cells.
Supporting Evidence for PRP
Despite skepticism, PRP’s efficacy is backed by extensive scientific research spanning decades and over 6000 studies. Patient willingness to pay out-of-pocket further underscores its perceived effectiveness, highlighting its growing popularity despite insurance coverage limitations.
Conclusion: Integrating PRP Into Practice
Choosing the right PRP kit is pivotal for optimizing treatment outcomes and patient satisfaction. With its proven benefits and increasing demand, integrating PRP into your medical practice offers a promising opportunity to enhance patient care and treatment efficacy.

- Published in Blog
Three popular PRP Treatments for Skincare
THURSDAY, 15 MARCH 2018 / PUBLISHED IN BLOG
Thousands of skincare centers across the nation provide at least one kind of PRP treatment. However, most do not go any further than micro-needling with a topical solution. This is mainly because it is far simpler than all other methods, and it is incredibly popular. However, it would make more sense for many practices that have invested in equipment to add PRP injections as well.
PRP Is Growing Substantially
Regardless of what is being treated, the protocol for obtaining PRP is the same: draw the blood, place it in the centrifuge, and then extract the PRP from the rest of the material. This simplicity, combined with PRP’s vast usability, can create significant and mind-blowing advances in modern medicine.
This includes skincare, as the PRP obtained from patients can be used in a plethora of ways. Here are a couple of examples of what can be performed by dermatologists and plastic surgeons worldwide.
Skin Augmentation
Adding a topical solution of PRP combined with microneedling can help regenerate dying skin cells and make the skin feel soft. Although this will probably work for most clients, many might want more. For instance, if you want to plump up the face, injecting PRP into the dermis can provide both beauty and a healing process.
If you want to create volume, you will need a filler. One way to do this is by using a Platelet-Poor Plasma filler (PPP), often left over from the PRP process. You can also use Hyaluronic Acid. A combination of these with PRP has been known to provide wonderful results, with some clinicians boasting a 100% success rate.
Vitiligo Correction
Many companies spend millions of dollars to find out how to turn defective cells healthy again, often looking into DNA technology. However, simply utilizing PRP may provide the same results. Some studies have shown that adding CO2 laser therapy for correcting vitiligo to a PRP treatment can increase its effectiveness by four times. This can also be beneficial in other areas, such as correcting wrinkles and even acne scars. So combining PRP treatments with conventional therapies can boost the effects tremendously.
If PRP can help boost the effects of lasers, it may also boost the effects of other skin therapies. This is a great opportunity to continue the work you do, but this time more effectively due to a simple method. Hundreds of skincare facilities are already providing this for their clients.
Hair Rejuvenation
Mesotherapy is a common treatment that utilizes microinjections to deliver medication throughout the skin’s surface. This procedure has provided great quality results by adding peptides and vitamins to the mix. However, one of the best ways to incorporate this into your practice is by using PRP therapy.
Mesotherapy can also be used to provide an even amount of PRP all over the body, including the face, neck, hands, etc. This helps to rejuvenate the skin and reduce wrinkles, discoloration, and stretch marks. However, it works best for hair loss treatments. In fact, adding PRP to mesotherapy has exceeded the industry’s expectations.
This is why PRP therapy is something every skincare clinic should offer. Since hair loss affects both men and women, it is important to make your treatments as effective as possible. Your patients will benefit from it, and satisfaction will rise. Is there any other reason to put it off?
“But I Never Heard Of Them!”
Some of these treatments and combinations are incredibly new, so new that many might not have heard of them before. This is why signing up to use them as soon as possible is vital. This way, you can be a step ahead of the competition when it comes to providing great services.
The demand for PRP is only growing over time, and the sooner you can get on board, the better off your practice will be. If you are interested in learning more about PRP therapy or checking out our line of PRP equipment, visit the Adimarket website.
PRP provides more effective treatments in less time, for less money, and with more satisfaction. Many practices have put their trust in this treatment and have been reaping the long-term benefits. PRP is here to stay. Are you ready to seize the potential of this great medical revolution.
- Published in Blog
- 1
- 2


![CartilageA[1]](https://www.issca.us/wp-content/uploads/2020/08/CartilageA1-460x260_c.jpg)