
MONDAY, 19 SEPTEMBER 2016 / PUBLISHED IN BLOG
Russian researchers have concluded that reprogramming does not create differences between reprogrammed and embryonic stem cells.
Understanding Stem Cells and Reprogramming
Stem cells are specialized, undifferentiated cells with the potential to develop into various cell types in the body. Pluripotent stem cells, capable of generating any cell type, are naturally found in early embryos. They are crucial for internal repair and growth during early life.
Reprogramming Techniques and Their Importance
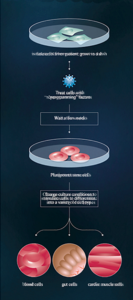
• Isolate cells from patient; grow in a dish •
Treat cells with “reprogramming”
• Wait a few weeks
• Pluripotent stem cells
• Change culture conditions to stimulate cells to differentiate into a variety of cell types
• blood cells | gut cells | cardio muscle cells
Credit: Moscow Institute of Physics and Technology
Reprogramming adult cells involves activating genes typically active in stem cells and deactivating those responsible for cell specialization. This pioneering work by Shinya Yamanaka, Nobel laureate, demonstrated that specific proteins could convert adult cells into pluripotent stem cells, known as induced pluripotent stem cells (iPSCs). This breakthrough avoids ethical concerns associated with using embryonic stem cells.
Potential Applications in Medicine
Stem cells hold promise for treating various diseases. Examples include transplanting retinal pigment epithelium and spinal cells, as well as regenerating teeth in mice. Reprogrammed iPSCs offer a revolutionary approach by allowing personalized treatment using a patient’s own cells.
Scientific Comparison: iPSCs vs. Embryonic Stem Cells
Recent studies have highlighted similarities and differences between iPSCs and embryonic stem cells. Researchers compared isogenic iPSC lines reprogrammed from different adult cell types previously derived from embryonic stem cells. Analysis of transcriptomes and methylated DNA areas showed comparable gene activity regulation mechanisms.
Research Findings and Implications
The study, published in the journal Cell Cycle, concluded that reprogramming adult cells into iPSCs does not leave distinguishing marks compared to embryonic stem cells. Differences observed were attributed to random factors rather than the reprogramming process itself.
“We defined the best induced pluripotent stem cell line concept,” says Dmitry Ischenko, Ph.D., researcher at the Moscow Institute of Physics and Technology.
Future Directions in Stem Cell Research

While this research doesn’t propose organ growth in vitro, it represents a crucial step toward understanding how specialized cells develop from pluripotent cells. Both iPSCs and embryonic stem cells offer potential for generating replacement cells and tissues to treat currently untreatable diseases.
Conclusion
The study, titled “An integrative analysis of reprogramming in human isogenic system identified a clone selection criterion,” involved researchers from the Vavilov Institute of General Genetics, Research Institute of Physical Chemical Medicine, and the Moscow Institute of Physics and Technology (MIPT).





