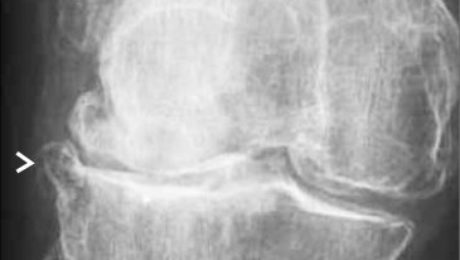
ISSCA to Host Conference in Mexico City.
ISSCA affiliates will share new research on clinical applications of stem cell treatments and provide tips on how to strategically grow a private practice.
MIAMI LAKES, Florida—The International Society for Stem Cell Application (ISSCA), a multi-disciplinary community of scientists and physicians collaborating to treat diseases and lessen human suffering through science, technology, and regenerative medicine, will host a two-day conference at the Hotel Barcelo Reforma in Mexico City. The event will take place on May 3-4, 2019 and will feature speakers from across the globe who are currently utilizing regenerative medicine in their medical practices.
Each day of the two-day conference will have a specific focus that will help attendees learn how to align their practices and methods with the regenerative medicine industry’s best practices by providing patients with safe stem-cell based therapies. Those attending will learn first-hand information about the science behind cell therapies and cell-based products. Additionally, conference registrants will learn how to distinguish between the most popular cellular products available on the market and which factors to consider when choosing stem cells as a therapeutic alternative.
Day one of the conference will feature lectures about regenerative medicine’s newest breakthroughs and focus on clinical applications of stem cell treatments using autologous stem cells and allogenic compounds such as cord blood and amniotic fluid from which to derive stem cells.

On the second day of the event, Mr. Benito Novas, Global Stem Cells Group CEO, will lead a lecture on the best marketing practices to strategically grow a private medical practice in the regenerative medicine sector and who to include in it. Some topics to be discussed include content marketing, social media management and Facebook and Google ads campaigns.
Over the two-day event, attendees will hear from eight speakers from six countries (US, Mexico, Costa Rica, Argentina, Bolivia and Cuba) discussing their experiences with using regenerative medicine to treat and heal their patients.
To learn more about the Mexico City conference and scheduled speakers, or to register, visit https://www.issca.us/certification-mexico/. To learn more about ISSCA and all of their upcoming and past events, visit https://issca.us/.
- Published in News
Global Stem Cells Group Invited to Speak at Jornadas Mediterraneas Conference.
ISSCA doctors to serve as keynote speakers at international conference and will host an additional stem cells course in Barcelona.
MIAMI LAKES, Florida— The International Society for Stem Cell Application (ISSCA), a multi-disciplinary community of scientists and physicians collaborating to treat diseases and lessen human suffering through science, technology, and regenerative medicine, has accepted an invitation to speak at the XXVIIas Jornadas Mediterraneas de Confrontaciones Terapeuticas en Medicina y Cirugia Cosmetica in Barcelona. The conference will be held on May 23-25, 2019 at the Hotel Barceló Sants, with experts from ISSCA leading the keynote session on May 25th. Following the conference on May 26th,, ISCCA doctors will also be hosting a one-day stem cells course for practitioners of regenerative medicine.
Dra. Maritza Novas of the United States and Dr. Leopoldo Parada of Chile will be speaking on behalf of ISSCA about new therapies based on allogenic compounds such as amniotic liquid, Wharton’s jelly, cord blood, and exosomes and how they present exciting new treatment opportunities for those practicing regenerative medicine.
Drs. Novas and Parada will shed light on new advances in allogenic compound research and share details with regenerative medicine practitioners on how allogenic compounds are safe treatment options for their patients, as they must pass through rigorous quality control in labs before being shipped to medical offices. Additionally, independent tests show that allogenic compounds have better cellular counts than other biological matter. Doctors currently using allogenic compounds have also reported faster treatment times associated with allogenic protocols, citing a 15-minute turnaround time versus 2 hours required to obtain stem cells from their patients.

After completing their keynote talk at Jornadas Mediterraneas, Drs. Nova and Parada will be leading a one-day stem cells seminar to discuss in further detail allogenic compound clinical applications and the latest clinical trials. The seminar will wrap up with a live patient demonstration.
ISSCA has attended Jornadas Mediterraneas for the last six years. It is a premier conference in the medical community attracting more than 500 doctors from across the globe each year.
To learn more about ISSCA and all of their upcoming and past events, visit https://issca.us/.
- Published in News
Global Stem Cells Group Continues to Expand Training Efforts in 6 International Cities
ISSCA’s training programs assist physicians and researchers in developing better protocols for stem cell treatments.
MIAMI LAKES, Florida— The International Society for Stem Cell Application, a multi-disciplinary community of scientists and physicians collaborating to treat diseases and lessen human suffering through science, technology, and regenerative medicine, is continuing to expand its global training efforts by sponsoring three upcoming training sessions over the next month. The group has a busy schedule, with trainings taking place in Amsterdam, Abu Dhabi, Atlanta, Bogota, Miami and Mexico City.
ISSCA instructors will be hosting two onsite trainings, one in Amsterdam, Netherlands on February 22-23 and another in Abu Dhabi, United Arab Emirates on March 2-3. The training is designed to assist physicians interested in introducing regenerative medicine into their practices adhere to industry practices. Physicians will learn about industry developments and the latest advances in cellular-based treatment protocols.
Utilizing ISSCA’s over 10 years of experience in regenerative medicine, the onsite trainings seek to bring the latest advances in the field to physicians across the world, removing barriers to access. In addition to training physicians, the group uses hands-on-training methods to instruct other medical staff in cellular treatment protocols so they can effectively assist their tending physicians. Trainings are highly personalized and offer physicians the ability to learn only the regenerative medicine treatments they are most interested in.
In early March, ISSCA instructors will also be traveling to Atlanta, Georgia to train physicians on allogenic compound stem cells derived from cord blood. This two-day training will take place in on March 29-30. Physicians with an interest in new regenerative medicine breakthroughs that have produced safer and shorter recovery times and those that have led to higher cellular counts in the degenerative disease treatment process will find this training of interest.
Instructors will lead physicians through a deep dive into the latest stem cell advances pertaining to cord blood research. Attendees will learn about processes for how to extract stem cells from a healthy donor and protocols on how to process stem cells in the lab while adhering to the highest quality control standards.
Instructors will additionally share the science behind allogenic compounds derived from cord blood and which current protocols use cord blood derived stem cells to promote patient healing.
ISSCA trainers will be rounding out their upcoming training schedule with visits to Bogota, Colombia on March 15-16, Miami, Florida on March 22-23 and Mexico City, Mexico on March 29-30. These three trainings will offer Stem Cell Training Certification for physicians seeking to expand their knowledge on the newest stem cells protocols for those wanting to integrate regenerative medicine into their practices. The protocols covered in the trainings can be implemented in medical offices with mini lab equipment. The instructors will engage physicians in hands-on instruction where doctors can practice on live patients.
Trainings in Bogota and Mexico City will be conducted in Spanish, and interested participants can find more information at www.cursocelulasmadre.com, while interested Miami participants can learn more at https://www.stemcelltraining.net/hands-on-course.
To learn more about ISSCA, visit https://www.issca.us/
- Published in News
Global Stem Cells Group to Host Stem Cells and Regenerative Medicine Conference in Miami
ISSCA to host upcoming regenerative medicine conference in Miami that provides training on allogeneic cellular-based products.
MIAMI LAKES, Florida—The International Society for Stem Cell Application, a multi-disciplinary community of scientists and physicians collaborating to treat diseases and lessen human suffering through science, technology, and regenerative medicine, is set to host a conference in Miami on October 25-26, 2019.
The conference will be held at the Biltmore Hotel and will offer more than 250 attendees the opportunity to learn more about allogenic cellular-based products and how they play a critical role in the future of regenerative medicine.

Physicians looking for new alternatives to improve the quality of life of their patients through emerging regenerative medicine protocols and advances are encouraged to attend the Miami conference. In this two-day event, attendees will learn why allogeneic cellular-based products have become today’s most popular regenerative medicine therapeutic option.
Well-respected scientists and researchers in the field of regenerative medicine from across the globe world will share with the audience the basic concepts needed to determine which allogenic cellular-based products are safe to use and what type of clinical indications can be targeted effectively.

“We are pleased to bring this informative and exciting conference to Miami,” said Benito Novas Global Stem Cells Group Founder and CEO. “Our goal is to give doctors the knowledge they need to begin implementing cellular-based treatments in their own practices. These types of treatments have been proven effective in a host of clinical scenarios, including speeding up the patient’s rate of recovery and pain management.”
To learn more about ISSCA, visit https://www.issca.us/
- Published in News
Opioid Overdose Crisis in America.
Let’s face it; it’s like America is missing it by paying more attention to Gun Violence murder and other deadliest diseases than opioid addiction that leads to an average number of deaths of 130 people every day. There is no doubt; the United States is in the midst of an opioid crisis, as overdose and addiction of opioids turns out to be a serious national crisis that has reduced the life expectancy of the US. With an average victim’s death hitting over 47,000 people recorded in 2017.
However, despite the alarming rate of death from opioid overdose, this problem is not grabbing the headlines from the media for health stakeholders to pay more attention and look for ways to finding lasting solutions to the anomaly.
It is worthy to note that, while many people are addicted to opioids in the form of heroin and synthetic opioids, millions of people are out there, taking an overdose of opioids in the form of pain reliever prescription for chronic pains and other related health issues. Though, opioids are used in the treatment of chronic pain, research has suggested that they may not help relieve pain in the long-term. This has posed a serious threat to public health and economic welfare, not only for the United States but other affected countries as well.
According to the Centers for Disease Control and Prevention, the total “economic burden” of only opioid misuse prescription in the US is estimated as $78.5 billion per year, inclusive of lost productivity, criminal justice involvement, healthcare cost, and addiction treatment.
This article aims to look at how we come to this point, some facts about opioids in the United States, and some useful information about opioid overdose. Read on to uncover them all.
Opioids and Substance Abuse at a Glance.
Opiates, popularly known as narcotics, are commonly prescribed for quick pain relief and sleep inducement. Originally, it is derived from poppy plant seeds or their byproducts. Opiates occur naturally in the form of opium and morphine, but most opiates are synthetic. These drugs became highly addictive because they create an intense sense of euphoria and as well as safeness, when adding it to pain-relieving properties.
Most patients with pain disorders later turn to rely on pharmaceutical opiates like oxycodone and hydrocodone; hence, they become addicted to it. However, opioid overdose has been studied to cause a number of health problems in the users, and these health issues are not limited to serious disorders, but even death. One of the prolonged effects of opioid usages is the brain’s inability to produce endorphins naturally. Endorphins are known to be the body’s natural painkillers.
Initially, around late 1990s, when opioids were becoming popular among the people, pharmaceutical companies came out to allay the fear of the people and reassure the medical community that opiate users would not become addicted to opioids prescribed for pain relief; hence, healthcare service providers started prescribing the drugs to patients at greater rates. Subsequently, this act resulted in a extensive misuse and diversion of these drugs prior to the time it was discovered that opioid prescriptions could actually be highly addictive like other opiates.
Facts about Opioid Prescription and Misuse in America.
The rates of opioid overdose in the United States started increasing in 2017 with over 47,000 citizens died due to misuse of opioids, such as heroin, prescription opioids, illicitly manufactured fentanyl (one of the powerful opioid synthetics). In the same year, this number was estimated 1.7 million and 652,000 Americans suffered from prescription opioid pain relievers and heroin use disorder respectively. The question is, how does it start?
It all starts when the body cannot properly manage and regulate pain again. In this condition, an opiate user may become addicted to the drugs, as the drugs now used to relief their pain and at the same time, create a sense of contentment and happiness in using them. Over time, even after the pains have gone, an opiate user will require more of the substance to reach the same level of high that creates happiness and contentment which they first experienced; hence, the person is already “an opiate addict.” Withdrawing from its use makes it even worse, as their bodies begin to show some unpleasant symptoms that make the user seeking more to relieve the symptoms.
From here, opioid prescription and misuse have turned out to become a public health problem in the United States with alarming rates of death on a daily basis.
Below are some facts about the opioid crisis in the United States:
- According to WQAD Digital Team’s claim of IMS Health’s market research, the number of opioid prescriptions doctors dispensed increased from 112 million to 282 million from 1992 to 2012 respectively. However, according to IQVIA, the number has declined to 236 million in 2016 and further dropped by 10.2% in 2017.
- Centers for Disease Control and Prevention, about 68% of cases of estimated 70,200 drug overdose deaths recorded in 2017 were linked to the use of opioids. This is more than six times compared to that of 1999 (including illegal opioids such as heroin and illicitly manufactured fentanyl and prescription opioids).
- According to a review, about 21 – 29% of patients with chronic pain who take opioids prescription misuse them.
- Another study also claimed that roughly 80% of heroin users initially misused prescription opioids.
- The same study also claimed that about 8 – 12% of opiate users develop an opioid use disorder.
- According to the Centers for Disease Control and Prevention, there is a 30% increase in opioid overdoses in 45 states of the United States between July 2016 to September 2017.
- In another review, opioid overdoses were seen increasing by 70% in the Midwestern region between July 2016 to September 2017.
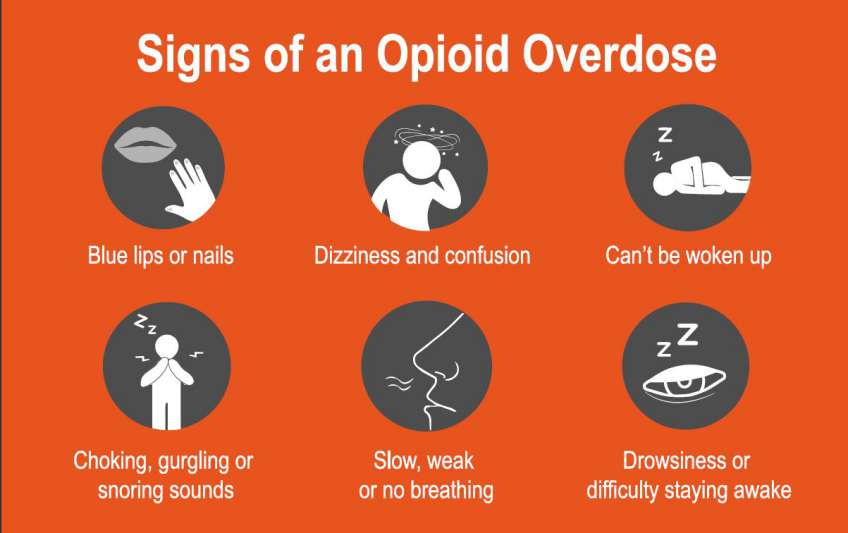
What is been doing about it?
With over two million opioid dependants in the United States, the U.S. Department of Health and Human Services (HHS) is making efforts to tackle the opioid crisis in America by focusing on five major areas. These include:
- Promoting and enlighten people on the use of overdose-reversing drugs.
- Giving people access to treatment and recovery therapies.
- Offering support for modern research on addiction and pain.
- Promoting public health surveillance to help people understand the epidemic better.
- Enhancing better pain management practices in the country.
In furtherance to the efforts of the U.S. Department of Health and Human Services (HHS), the National Institutes of Health (NIH)’s Director Francis S. Collins in April 2018’s National Rx Drug Abuse and Heroin Summit, announced the launch of a special program referred to HEAL (Helping to End Addiction Long-term) Initiative. HEAL is an aggressive effort set up to expedite scientific solutions to address the opioid crisis in the United States.
Final Words.
Just because media are not paying attention to the opioid crisis in the US does not mean things are working in the medical world. With the alarming rate of opioid overdose and an increasing number of Americans abusing prescription and becoming dependent on opioids, all hands must be on deck to find a lasting solution to the current problem. While different agencies and stakeholders are not relenting on their efforts, more medical developments and approaches are still required to achieve a good result.
- Published in Blog
Autologous mesenchymal stem cell application for cartilage defect in recurrent patellar dislocation: A case report
Introduction.
Recurrent patellar dislocation is a repeated dislocation that follows from an initial episode of minor trauma dislocation . Conservative management gives a minimal result in re-dislocation, with persistent symptoms of anterior knee pain, instability and activity limitation. Meanwhile, there is no gold standard treatment of realignment procedures. This can further cause cartilage lesion in the patella and femoral condyle, and consequently increase the risk of re-dislocation. Mesenchymal stem cells (MSCs) have been widely explored for treating cartilage defect due to their potency of chondrogenic differentiation. We present a novel approach of treating cartilage lesions in recurrent patellar dislocation by combining of arthroscopic microfracture and autologous bone marrow derived MSCs (BM-MSCs) after Fulkerson osteotomy.
Presentation of case.
A 21-year-old male presented with left knee discomfort. Ten years ago, the patient felt discomfort on the medial side of the knee and felt his knee cap slide out laterally. The patient experienced several episodes of instability ranging from a feeling of “giving away” until a prominent lateral sliding-off of his knee cap. Anterior knee pain has also occurred during activities such as climbing stairs or exercising.
Physical examination revealed slight pain on the anterior side of the patella, but no atrophy or squinting patella. Knee range of motion (ROM) was normal when the knee cap position was normal, but was limited when it was dislocated (0–20°). Lateral subluxation of the patella was found when the knee was extended from 90° flexion position (J-sign positive), positive patellar apprehension test, with medial patella elasticity/patellar glide >2 quadrants. The Q angle, in the 90° flexed knee position, was 10°, which was still normal. The plain radiograph imaging showed no abnormality. Insall-Salvati index was 1.12. The patient was diagnosed with recurrent patellar dislocation, with suspected cartilage lesion of the left knee.
The first surgery was an arthroscopy diagnostic and distal realignment procedure (lateral retinaculum release, percutaneous medial retinaculum plication, and antero-medialization of tibia tubercle/Fulkerson osteotomy). We found articular cartilagedefects on the lateral condyle of the femur with a diameter of 3 cm (Figure. 1A), and on the postero-medial with a diameter of 2.5 cm (Figure. 1B), and the depth of both was more than 50% of the cartilage thickness. We determined that the articular defect was Grade 3 according to International Cartilage Regeneration & Joint Preservation Society (ICRS). We performed a dissection of lateral retinaculum (lateral release) (Figure. 1C) using an electrocautery, continued by incising the medial side of tibia tuberosity and detaching the patellar tendon by using an oblique osteotomy procedure on tibia tuberosity, where the fragment slide 1 cm antero-medially and fixed with two 3.5 mm (length 40 mm) partial threaded cancellous screw, followed by percutaneous plication on the medial side of the patella using non-absorbable string (Figure. 2A). Post-operative ROM was 90° flexion without any dislocation (Figure. 2B) and the position of the screws was good (Figure. 2C).

Figure 1.A. Cartilage defect on the femoral lateral condyle with a diameter of 3 cm (pointed by the arrow). B. Articular cartilage defect on posteromedial patella with a diameter of 2.5 cm (pointed by the arrow). C. Lateral retinaculum dissection/lateral release using an electrocautery (pointed by the arrow).

Figure 2.A. Percutaenous medial plication using non-absorbable string no.2. B. Post-operative anteroposterior and lateral projection of plain radiograph imaging. C. Post-operative CT scan.
One month after surgery, full ROM and weight bearing exercises were started, including knee exercise until maximum flexion was reached along with quadriceps muscle exercise. Eighteen month after that surgery, we performed an iliac crestbone marrow aspiration; arthroscopic microfracture by using an awl until 4 mm depth was reached on the site located ±3–4 mm from the articular cartilage defect on the posteromedial patella and femoral lateral condyle (Fig. 3A); and tibial tuberosity screw removal.

Figure 3.A. Arthroscopic microfracture on cartilage defect using an awl, with a depth of ±4 cm. B. The mesenchymal stem cell culture after day 22 showing fibroblast-like cell/spindle shaped cells that 100% confluent.Approximately 30 mL of bone marrow was aspirated from the posterior iliac crest. Bone marrow aspirate was diluted in phosphate-buffered saline (PBS) and centrifuged at room temperature. The buffy coat was washed and cultivated for 3–4 weeks until reaching the required amount (107 MSCs/mL) (Figure. 3B). The cells were harvested and characterized with flow cytometer. The MSCs, having negative bacteria and fungi tests, were injected intra-articularly into the left knee. Then, 2 mL HA were injected weekly for 3 weeks. Non-weight bearing exercise was conducted for 6 weeks.
Outcomes were assessed by using International Knee Documentation Committee (IKDC) score, visual analog scale (VAS) score and imaging. Baseline IKDC score was 52.9 and VAS score was 8. Nineteen months after the first surgery, IKDC score was improved to 93.1, while the VAS score decreased to 2. Six months after MSCs implantation, evaluation by MRI FSE cor T2-weighted signal (cartilage sequence) showed a significant growth of articular cartilage covering most of the defect (Figure. 4). Two years after the MSCs implantation, there was no complaint and full ROM was reached.

Figure 4.MRI FSE cor T2-weighted signal in different slice. Left image showing cartilage defect (pointed by the arrow). Right image showing cartilage growth was found in the defect (pointed by the arrow).
Discussion
Recurrent patellar dislocation are uncommon problem, with recurrence rate 15%–44% after conservative management, while cartilage lesions following recurrent patellar dislocations are quite common, but still no gold standard or consensus on the management. This patient was diagnosed as chondromalacia Grade 3 Outerbridge classification and Grade 3 ICRS. One of the suitable procedures for recurrent patellar dislocation with chondromalacia, especially Grade 3 or 4, was Oblique Fulkerson-type osteotomy, with or without the release of lateral retinaculum. This distal realignment procedure could decrease patellofemoral pain by anteriorization of tibial tuberosity, decreasing articular contact pressure and at the same time medializing knee extensor mechanism. Therefore, we performed the Fulkerson-type osteotomy with lateral retinacular release, combined with percutaneous medial plication since the patient was already 21 years of age and the bone was expected to be mature so that the risk of premature physeal closure in proximal tibia can be avoided. This technique has demonstrated good results (86%), although it had a risk of tibial stress fracture in the healing process. The lateral retinacular release is an adjuvant after tibial tubercle medialization to re-center the patella. It was reported that isolated lateral retinacular release significantly gives an inferior long-term result compared to medial reefing. Percutaneous plication of medial patella procedure was indicated to build a strong construct by shortening the patellofemoral ligament, in order to prevent lateral sliding of the patella.
Treatment of articular cartilage defect remains challenging since it has limited self-healing capacity. Lesions that do not reach the subchondral zone will be unlikely to heal and usually progress to a cartilage degeneration. Limited blood supply in the cartilage and low chondrocyte metabolic activity disrupt natural healing that is supposed to fill the defect by increasing hyaline cartilage synthesis activity or stem cell mobilization from bone marrow to site of injury. The proper initial procedure for chondral lesion >4 cm2 was marrow stimulation by mosaicplasty or microfracture; and for a lesion <4 cm2 and >12 cm2 accompanied with symptoms, autologous cartilage implantation (ACI) beneath a sutured periosteal flap was promising. This procedure could not regenerate cartilage in the long term, due to loss of flap or cell suspensions. A scaffold (e.g. HA) was then used to act as an anchorage for chondrocytes adherence on cartilage defects and to promote the secretion of chondrocyte extracellular matrix. The BM-MSCs implantation could be an alternative source of the chondrocytes. Human BM-MSCs are relatively easy to isolate and to be cultured in such a condition that may retain their capability to differentiate into chondrocytes.
The MSCs effect was reported as effective as ACI and even had the advantage over ACI in terms of the number cells obtained, better proliferation capacity and less damage in the donor site. Treating large cartilage defects by using BM-MSCs showed good outcome, but the transplantation procedure was invasive. Wong et al. conducted a clinical study of the BM-MSCs intra-articular injection in combination with high tibial osteotomy (HTO) and microfracture for treating cartilage defect with varus knee. They reported that intra-articular MSCs injection improved the outcomes in the patients undergoing HTO and microfracture. Here we performed also a less invasive approach by injecting the autologous BM-MSCs intra-articularly, following the arthroscopic microfracture using an awl to penetrate the subchondral bone plate in the cartilage defects, which led to clot formation. This clot contains progenitor cells, cytokines, growth factors and pluripotent, marrow-derived mesenchymal stem cells, which produce a fibrocartilage repair with varying amounts of type-II collagen content. Cytokine within the fibrin clot will attract the injectable stem cells to the cartilage lesions.
The HA injection in this patient was aimed to suspend the MSCs and to support regenerative potency of MSCs with chondroinductive and chondroprotective potency of HA. Intraarticular injection of MSCs suspended in HA could be an alternative treatment for large cartilage defect. Supporting microfracture technique by intra-articular HA injections had a positive effect on the repair tissue formation within the chondral defect. The MRI showed that there was a growth of articular cartilage covering most of the defect even though it was not perfect as yet.
Conclusion
This case report demonstrated that combining Fulkerson osteotomy with the lateral retinacular release and percutaneous medial plication was effective in treating chronic patellar instability. The combination of microfracture and MSCs implantation was safe and could regenerate the articular cartilage in this patient.
- Published in Blog
Autologous micro-fragmented adipose tissue for the treatment of diffuse degenerative knee osteoarthritis: an update at 3 year follow-up
Background.
The management of chondral disease is challenging because of its intrinsic poor healing potential. Biomechanical and biological changes may lead to the loss of tissue homoeostasis, resulting in an accelerated degeneration of the articular surface, eventually leading to end-stage osteoarthritis (OA).
Conservative therapies for the treatment of knee degenerative processes, such as non-pharmacological interventions, systemic drug treatment and intra-articular therapies are used before resorting to surgery; nonetheless, they may offer only short-term benefits. Encouraging preliminary results have been reported using mesenchymal stem cells (MSCs), either alone or in association with surgery. Among the many sources of MSCs, adipose tissue has created a huge interest in the context of cartilage regeneration (Pak et al. 2016; Ruetze and Richter 2014), due to its wide availability, ease to harvest and richness in mesenchymal cell elements within the so called stromal vascular fraction (De Girolamo et al. 2016; Caplan 2008; Caplan and Correa 2011; Caplan and Dennis 2006). Moreover, MSCs from adipose tissue are characterized by marked anti-inflammatory and regenerative properties, which make them an excellent tool for regenerative medicine purposes (De Girolamo et al. 2016; Caplan 2008; Caplan and Correa 2011; Caplan and Dennis 2006). Nevertheless, preparation of autologous MSCs for injection requires ex vivo culture from a good manufacturing practice facility, which makes the process laborious and expensive (Ährlund-Richter et al. 2009; Arcidiacono et al. 2012; Sensebé et al. 2010). An increasing number of adipose tissue-derived cell isolation systems, allowing for minimal manipulation, have been developed in the last years. We previously reported the safety and feasibility of autologous micro-fragmented adipose tissue as adjuvant for the surgical treatment of diffuse degenerative chondral lesions at 1 year follow-up (Russo et al. 2017). Here we present the outcomes of the same cohort of patients evaluated at 3 year follow-up.
Methods.
The original study was approved by the Ethics Committee of Verona and Rovigo – Italy (protocol n° 10,227, March 1st, 2016). An extension of the study protocol has been conceded by the same authority to evaluate the results at 3 years (protocol n° 14,505, March 14th 2018) and written informed consent was obtained from all patients.
Study design and population, surgical techniques, post-op rehabilitation protocol, safety and clinical evaluation were previously described (Russo et al. 2017). Briefly, 30 patients, affected by diffuse degenerative chondral lesions of different degrees of severity, were treated with autologous and micro-fragmented adipose tissue between 1stJanuary 2014 and 31st December 2014. Of these 30 patients, 24 (80%) also had an associated surgery (ACL/LCL reconstruction, high tibial osteotomy, meniscectomy), while six (20%) underwent arthroscopy alone. For the 3 year follow-up all the patients were re-contacted and clinically evaluated by the same clinicians.
Findings.
Of the 30 patients treated with autologous micro-fragmented adipose tissue, eight also had meniscal surgery, five plate removal, three osteotomy, two ligament surgery, two microfractures, and four other surgical procedures. The remaining six had arthroscopy alone. Despite the heterogeneity of the associated surgical procedures all the patients shared the presence of chondral lesions of different degrees of severity (Russo et al. 2017).At 3 years follow-up, one patient was lost, and seven (23%) received additional treatments in the period of observation, and therefore have been considered failures. In detail, between 18 and 30 months, one patient had three injections of hyaluronic acid and the other six had multiple injections of platelet rich plasma. Background data on this subpopulation is reported in Table 1.
Table 1: Background data of the failures (n = 7)
| Age y/o | |
| Mean | 36.3 |
| Standard deviation | 7.3. |
| Type chondropathy | |
| FC | 4 (57%) |
| TP | 2 (29%) |
| PF | 6 (86%) |
| Three-compartment | 2 (29%) |
| Associated surgery | |
| YES | 5 (71%) |
| NO | 2 (29%) |
FC femoral condyle, TP tibial plateau, PF patellofemoral.
No adverse events, lipodystrophy cases at the harvesting site nor atypical inflammatory reactions at the joint level were reported in the 3 year period for all the 29 patients.On average, the 22 patients that had no other treatments in the 3 year period (Table 2) showed that the results observed at 1 year were maintained (T36 vs. T12, p > 0.05). Moreover, 41, 55, 55 and 64% of the patients improved with respect to the 1-year follow-up in the Tegner Lysholm Knee, VAS, IKDC-subjective and total KOOS, respectively.
Table 2: Background data of the population (n = 22)
| Age y/o | |
| Mean | 44.7 |
| Standard deviation | 11.4 |
| Gender | |
| M | 14 (64%) |
| F | 8 (36%) |
| BMI | |
| Mean | 25.9 |
| SD | 3.3 |
| Sport | |
| Profesionals | 1 (4%) |
| Amateurs | 9 (41%) |
| Occasional | 5 (23%) |
| Inactive | 7 (32%) |
| Grade chondropathy (ICRS classification) | |
| II | 7 (32%) |
| III | 6 (27%) |
| IV | 9 (41%) |
| Type chondropathy | |
| FC | 17 (77%) |
| TP | 14 (64%) |
| PF | 14 (64%) |
| Three-compartment | 9 (41%) |
| Associated surgery | |
| Yes | 18 (82%) |
| No | 4 (18%) |
FC femoral condyle, TP tibial plateau, PF patellofemoral. Compared to pre-operative values, more than 50% of the patients improved at least 20 points in all the considered scores, and, surprisingly, 55% of the patients improved at least 30 points in the VAS pain scale.
A summary of the results is reported in Figure 1.

Figure 1: Trend of functional improvements of Tegner Lysholm knee, VAS pain, IKDC subjective and total KOOS pre-operatively (white bars), at 12 (grey bars) and 36 months (black bars) after micro-fragmented adipose tissue injection. Results are expressed as mean and standard error.
Discussion
The main finding of this study is that the beneficial effect of autologous micro-fragmented adipose tissue as adjuvant for the treatment of diffuse degenerative chondral lesions is maintained in the mid-term. In addition, no complications were observed in the 3 year period showing the safety profile of this procedure. No patient, including the seven patients who received additional treatments, worsened compared to the pre-operative condition.
Despite the heterogeneity of the associated surgical procedures all the patients shared the presence of chondral lesions of different degrees of severity, which may have been responsible for the impairment in function and pain.
As reported in literature, articular surface damages, especially when diffused (three compartment OA), positively correlate with a decay in the outcomes in patients who received knee surgery for other reasons (Bonasia et al. 2014; Røtterud et al. 2012; Saithna et al. 2014; Su et al. 2018; Verdonk et al. 2016). Published data shows a decline in the clinical results in the mid to long-term for arthroscopic and chondral debridement procedures in cases of initial knee OA (Su et al. 2018). Some authors assessed the effectiveness of the arthroscopic or conservative treatments in patients diagnosed with knee OA (Kellgren-Lawrence grade 2 to 4) with 5 years of follow-up, concluding that arthroscopy provided no benefit in decreasing or delaying arthroplasty and that it can relieve symptoms only up to 2 years (Su et al. 2018). The same observation has been reported for ligament reconstruction, where the short and mid to long-term benefits are inferior in patients who have cartilage lesions. In a study of a cohort of ACL-injured patients with full-thickness cartilage lesions (ICRS grade III–IV), the authors showed that ACL-injured patients with full-thickness cartilage lesions reported worse outcomes and minor improvement after ACL reconstruction compared to patients without cartilage lesions at 2–5 years follow-up, although no significant differences between the two groups at the time of ACL reconstruction were present. This means that the observed differences between the groups must have occurred during the follow-up period (Røtterud et al. 2012). Furthermore, the outcomes of osteotomy procedures in patients with diffuse degenerative knee chondropathy worsen in the mid to long-term (Bonasia et al. 2014; Saithna et al. 2014). In a study reporting the results of a case series of opening wedge distal femoral varus osteotomies for valgus lateral knee OA, it is shown that re-operation for non-arthroplasty related surgery was common due, besides others, to infection and persistence of symptoms (Saithna et al. 2014). With regard to meniscectomy, in a recently published paper it is concluded that meniscus therapy including partial meniscectomy, meniscus suture, and meniscus replacement has proven beneficial effects in long-term studies in patients without cartilage damage, supporting the hypothesis that meniscectomy increases the risk of cartilage degeneration (Verdonk et al. 2016).
Based on the aforementioned published evidences, we should have expected, in the mid-term, a decay of the outcomes. Notably, the results have been maintained with no significant differences in all the evaluated parameters with respect to the 1 year follow-up assessment. Furthermore, in line with that already observed at 1 year, the patients with lesions in more than one compartment had higher and statistically significant improvements compared to patients with lesions in only one compartment (p < 0.01). This finding supports our hypothesis of using micro-fragmented adipose tissue for the treatment of the diffuse degenerative knee pathology as an adjuvant of the surgical procedures. Indeed, the maintenance of stable results at the last follow-up leads to hypothesize a protective role of micro-fragmented adipose tissue in a further chondral degeneration.
The seven patients who received additional biological therapies in the 3-year period, were young (mean age 36.3 ± 7.3 vs. 44.7 ± 11.4), very active in sport and 6 out of 7 had a patellofemoral chondropathy. Their conditions after 1 year did not worsen, but they probably needed an additional biological treatment because of their high functional demands and the presence of the patellofemoral chondropathy, which is a negative prognostic element, even if the small number of patients does not allow for any statistical correlation.
References.
- Ährlund-Richter L, De Luca M, Marshak DR, Munsie M, Veiga A, Rao M (2009) Isolation and production of cells suitable for human therapy: challenges ahead. Cell Stem Cell 4(1):20–26View ArticleGoogle Scholar
- Arcidiacono JA, Blair JW, Benton KA (2012) US Food and Drug Administration international collaborations for cellular therapy product regulation. Stem Cell Res Ther 3(5):1View ArticleGoogle Scholar
- Bonasia DE, Dettoni F, Sito G, Blonna D, Marmotti A, Bruzzone M, Castoldi F, Rossi R (2014) Medial opening wedge high tibial osteotomy for medial compartment overload/arthritis in the varus knee: prognostic factors. Am J Sports Med 42(3):690–698View ArticleGoogle Scholar
- Caplan AI (2008) All MSCs are pericytes? Cell Stem Cell 3(3):229–230View ArticleGoogle Scholar
- Caplan AI, Correa D (2011) The MSC: an injury drugstore. Cell Stem Cell 9(1):11–15View ArticleGoogle Scholar
- Caplan AI, Dennis JE (2006) Mesenchymal stem cells as trophic mediators. J Cell Biochem 98(5):1076–1084View ArticleGoogle Scholar
- De Girolamo L, Kon E, Filardo G, Marmotti A, Soler F, Peretti G, Vannini F, Madry H, Chubinskaya S (2016) Regenerative approaches for the treatment of early OA. Knee Surg Sports Traumatol Arthrosc 24(6):1826–1835View ArticleGoogle Scholar
- Pak J, Lee JH, Kartolo WA, Lee SH (2016) Cartilage regeneration in human with adipose tissue-derived stem cells: current status in clinical implications. Biomed Res Int 2016:4702674View ArticleGoogle Scholar
- Røtterud JH, Risberg MA, Engebretsen L, Årøen A (2012) Patients with focal full-thickness cartilage lesions benefit less from ACL reconstruction at 2–5 years follow-up. Knee Surg Sports Traumatol Arthrosc 20(8):1533–1539View ArticleGoogle Scholar
- Ruetze M, Richter W (2014) Adipose-derived stromal cells for osteoarticular repair: trophic function versus stem cell activity. Expert Rev Mol Med 16:e9View ArticleGoogle Scholar
- Russo A, Condello V, Madonna V, Guerriero M, Zorzi C (2017) Autologous and micro-fragmented adipose tissue for the treatment of diffuse degenerative knee osteoarthritis. J Exp Orthop 4(1):33View ArticleGoogle Scholar
- Saithna A, Kundra R, Getgood A, Spalding T (2014) Opening wedge distal femoral varus osteotomy for lateral compartment osteoarthritis in the valgus knee. Knee 21(1):172–175View ArticleGoogle Scholar
- Sensebé L, Bourin P, Tarte K (2010) Good manufacturing practices production of mesenchymal stem/stromal cells. Hum Gene Ther 22(1):19–26View ArticleGoogle Scholar
- Su X, Li C, Liao W, Liu J, Zhang H, Li J, Li Z (2018) Comparison of arthroscopic and conservative treatments for knee osteoarthritis: a 5-year retrospective comparative study. Arthroscopy 34(3):652–659View ArticleGoogle Scholar
- Verdonk R, Madry H, Shabshin N, Dirisamer F, Peretti GM, Pujol N, Spalding T, Verdonk P, Seil R, Condello V (2016) The role of meniscal tissue in joint protection in early osteoarthritis. Knee Surg Sports Traumatol Arthrosc 24(6):1763–1774View ArticleGoogle Scholar
- Published in Blog
- 1
- 2